Anticipation, excitement, love, and nervousness are natural emotions when bringing a new life into the world. It is a time that can also bring concern and uncertainty along the way for parents.
One of the worries many parents may face is the possibility of their child being born with a birth defect or congenital abnormality.
According to the CDC, birth defects affect one in every 33 babies (about 3% of all babies) born in the United States annually.
While these conditions can be challenging to comprehend, understanding birth defects and their associated risk factors can help parents navigate their prenatal and postnatal concerns.
Below, we’ll discuss everything you need to know – what birth defects are, what it’s like to manage and live with these conditions, and answer common questions surrounding the following birth defects or congenital abnormalities:
- Congenital Heart Defects
- Cleft Lip and Cleft Palate
- Down Syndrome
- Neural Tube Defects
- Clubfoot
What Are Birth Defects?
Birth defects, often called congenital abnormalities, are structural or functional anomalies affecting various body parts.
Know that birth defects vary widely in severity, and their impact on a child’s life can range from mild to significant. The heart, brain, limbs, and organs can all be affected depending on the condition.
Below are a few of the most common birth defects or congenital abnormalities broken down into a description, understanding of the causes, treatment options, and more.
Common Birth Defects
Congenital Heart Defects
Congenital heart defects (CHDs) are among the most common birth defects, affecting approximately 1 in every 110 newborns worldwide.
This condition involves a range of structural and functional abnormalities present at birth in the heart or the blood vessels near the heart.
Causes
The causes of congenital heart defects can be multifaceted. Some result from genetic factors; however, only 15-20% of all CHDs are related to known hereditary conditions.
Other causes may link to maternal infections during pregnancy, exposure to certain medications or substances, or remain unexplained.
It’s worth noting that a baby’s risk of CHD is three times more likely if the family, such as the mother, father, or sibling, has a CHD.
Risk Factors for Congenital Heart Defects
- Genetics: A family history of CHD can increase the risk.
- Maternal Infections: Infections like rubella during pregnancy can elevate the risk.
Treatments
Treatment options for congenital heart defects vary and can include medication or surgical interventions, depending on the specific condition.
The key to improving outcomes is early diagnosis and timely intervention.
Living with Congenital Heart Defects
Understand that congenital heart defects may require ongoing medical care and lifestyle adjustments.
Many individuals with CHD lead active lives, but following a healthcare provider’s guidance and attending regular check-ups is essential.
Common Questions On Congenital Heart Defects
- Q: What is the long-term outlook for a child with a congenital heart defect?
- A: The long-term outlook varies depending on the specific CHD and its severity. People with CHD can lead healthy and fulfilling lives with proper medical management and follow-up care.
- Q: Can children with congenital heart defects participate in sports and physical activities?
- A: In many cases, children with CHD can participate in sports and physical activities under the guidance of a healthcare provider. The level and extent of participation allowed will also be determined by a healthcare professional.
Sources: Children’s Heart Foundation
Cleft Lip and Cleft Palate
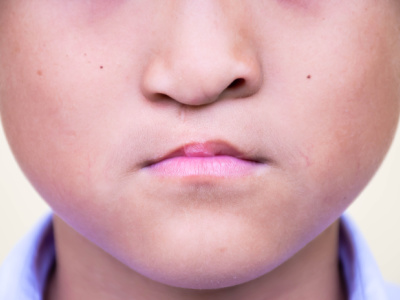
Cleft lip and cleft palate are congenital conditions characterized by openings or splits in the upper lip (cleft lip) or the roof of the mouth (cleft palate).
Affecting approximately 1 in 600 newborns each year – Cleft lip and palate are some of the most common birth defects.
Causes
The exact causes of cleft lip and palate are not always straightforward. However, causes may result from a combination of genetic and environmental factors.
According to the American Cleft Palate Craniofacial Association (ACPA), Cleft lip is most common among people of Native American and Asian ancestry. It is least common in those of African ancestry.
Risk Factors for Cleft Lip and Cleft Palate
- Genetics: A family history of cleft lip or palate increases the risk.
- Maternal Smoking: Smoking during pregnancy is associated with a higher risk.
Treatments
Typically performed in infancy, surgical repair via a craniofacial team can correct cleft lip and palate.
Living with Cleft Lip and Cleft Palate
A craniofacial professional usually performs surgery to close a cleft lip within the first few months of life.
For babies born with cleft palate, surgery will take place a couple of months later, and usually endure additional operations throughout their early stages of life.
It’s best to meet with a professional craniofacial team for a better understanding!
Common Questions On Cleft Lip and Cleft Palate
- Q: Can individuals with cleft lip and cleft palate lead everyday lives?
- A: Many individuals with cleft lip and palate lead everyday lives with proper medical care and support. Early intervention and ongoing medical management are crucial.
Sources: American Cleft Palate-Craniofacial Association
Down Syndrome

Down syndrome is a genetic condition caused by an extra chromosome 21 in cells. This condition occurs in about 1 in 772 births – the most common chromosomal disorder.
People with Down Syndrome have intellectual and developmental disabilities, which range from mild to severe.
However, people with Down syndrome are becoming increasingly involved in everyday life!
Causes
As mentioned, down syndrome is caused by having an extra chromosome 21. 95% of Down syndrome cases stem from an error in cell division. This error is called nondisjunction.
According to the National Down Syndrome Society, Nondisjunction results in an embryo with three copies of chromosome 21 instead of two.
A pair of the 21st chromosomes in either the sperm or egg fail to separate before conception, resulting in replicated extra chromosomes through every cell in the body.
Risk Factors for Down Syndrome
- Maternal Age: Age is the only factor linked to higher chances of having a child with Down Syndrome. Environmental and prenatal factors and full-term parental activities are also not scientifically related to Down Syndrome.
Treatments
Early intervention programs focusing on speech and language development, motor skills, and cognitive abilities can significantly benefit children with Down syndrome.
Regular medical check-ups and clinical treatments are essential to address potential health issues.
Living with Down Syndrome
Individuals with Down syndrome can lead long, fulfilling lives with the proper support and resources.
With advancements in treatments, as many as 80% of adults with Down syndrome reach age 60.
Early intervention programs, educational support, and healthcare are essential for maximizing their potential.
Many people with Down syndrome are active in their communities and may pursue employment and independent living.
Common Questions on Down Syndrome
- Q: What are the educational options for children with Down syndrome?
- A: With many resources available, children with Down syndrome benefit from early intervention programs and inclusive education programs reaching primary, secondary, and higher education students.
- Q: What is the life expectancy for individuals with Down syndrome?
- A: Life expectancy for individuals with Down syndrome has significantly increased. Many people with Down syndrome now live into their 60s and 70s with proper medical care and a healthy lifestyle.
Sources: National Down Syndrome Society
Neural Tube Defects
Neural tube defects (NTDs) occur when the neural tube, responsible for forming the baby’s brain and spinal cord, does not close properly during a baby’s early development stages.
Spina Bifida and Anencephaly
Approximately 3,000 cases occur yearly in the United States, with Spina Bifida and Anencephaly among the most common conditions.
Spina Bifida occurs when the spinal cord extends through the spine due to the spine’s bones not fully closing.
This condition can lead to paralyzed legs and bladder and bowel control difficulties in affected children.
However, Some cases are milder and may have fewer complications.
Anencephaly is a severe Neural tube defect resulting from incomplete closure of the upper part of the neural tube.
Significant brain, skull, and scalp abnormalities stem from this condition. Sadly, babies born with anencephaly typically survive only a few hours after birth.
Causes
The cause of NTDs is unknown; however, experts believe a combination of genetic and environmental factors can contribute to these conditions.
Risk Factors for Neural Tube Defects
- Folic Acid Intake: Inadequate folic acid intake during pregnancy increases the risk. According to the Centers for Disease Control and Prevention (CDC), taking 400 micrograms (mcg) of folic acid daily can help prevent Neural tube defects.
Treatments
Spina Bifida may require a specialized care team to perform an initial spinal repair surgery.
From here, daily physiotherapy and occupational therapy can help with day-to-day activities and reaching independence.
Anencephaly is a severe condition with no known treatments, and unfortunately, it is not compatible with life.
Living with Neural Tube Defects
Living with a neural tube defect can be challenging and requires ongoing medical care and support.
In seeking independence, physical therapy and assistive devices can help improve mobility for those with spina bifida
Common Questions on Neural Tube Defects
- Q: Can children with spina bifida lead active lives?
- A: With the proper medical care and support, children with spina bifida can lead active and fulfilling lives. Physical therapy and assistive devices are often part of their management.
- Q: What is the prognosis for an infant with anencephaly?
- A: Anencephaly is a severe condition with a poor prognosis. Most infants with anencephaly do not survive long after birth.
Sources: March of Dimes, NHS
Clubfoot

Clubfoot is a congenital deformity that affects one or both feet, causing them to point inward and downward. It is a common congenital condition affecting around every 1 in 1000 births.
According to the Academy of Orthopedic Surgeons, It is a condition where the tendons linking leg muscles to the foot bones are short and tight, leading to a severe inward turn of the foot.
While clubfoot is diagnosed at birth, prenatal ultrasounds can also detect it.
Causes
The exact cause of clubfoot is unclear but may involve genetic factors or abnormal positioning in the womb.
Risk Factors for Clubfoot
Genetics are likely to play a role in risk factors for clubfoot; however, it is unclear which genes are responsible for this condition.
It is worth noting that gender, neuromuscular disorders, and other birth defects are considered to be risk factors.
Treatments
Clubfoot can often be successfully corrected with casting, stretching, and bracing procedures, typically initiated shortly after birth through specific methods. The goal of clubfoot care is normal growth in tendons, bones, and muscles.
Regular follow-up with orthopedic specialists is crucial to monitor progress and address potential issues.
Living with Clubfoot
With early intervention and proper treatment, most children with clubfoot can achieve normal mobility and lead active lives!
Know that clubfoot does not get better if left alone, so early treatments and bracing are key with regular follow-ups with orthopedic specialists.
Common Questions on Clubfoot
- Q: Can clubfoot be corrected without surgery?
- A: Clubfoot is corrected without surgery through casting and stretching procedures. Surgery is usually reserved for cases that do not respond to non-surgical treatments.
- Q: Will my child have long-term mobility issues due to clubfoot?
- A: With appropriate treatment and follow-up care, most children with clubfoot can achieve normal mobility and lead active lives.
Sources: American Academy of Orthopaedic Surgeons, Boston Children’s Hospital
Final Thoughts
Through every emotion in your parenthood journey, know you are not alone.
At Cool Springs Obstetrics and Gynecology, we understand that the mother and baby’s health and well-being are paramount during pregnancy and postpartum.
While we no longer provide obstetrics care, be assured that our team is board-certified by The American Board of Obstetrics and Gynecology.
To ensure that you receive the best possible obstetric care, we are pleased to offer referrals to exceptional obstetricians within Dr. Lodge’s network. These referrals are based on your specific needs and preferences.
Serving Brentwood, Franklin, and surrounding Nashville areas, we are dedicated to guiding you in making informed choices and ensuring you receive the highest quality of care during this phase of life.