Genital warts are growths that can appear on or around the genitals after contracting a sexually transmitted infection (STI) that is caused by certain strains of the human papillomavirus (HPV). While the HPV that causes genital warts is extremely common, symptoms are not.
Many people who have the HPV that causes genital warts are asymptomatic and never develop visible growths. For those who do get warts, it could be months or even years after becoming infected before they appear. This can lead many women to mistake the typically small, painless growths for other common skin conditions, like razor burn. Or, cause stress, thinking it could be a more serious STD like genital herpes, or a more rare bump that some people call a nodule of gonorrhea.
Because the HPV that causes genital warts is so common, yet often misunderstood, and many people don’t realize that it can be spread from skin-to-skin sexual contact (meaning condoms aren’t always enough to protect you from the HPV virus), having clear and accurate information about genital herpes from an OBGYN that diagnoses and treats STIs is essential for your health and the health of your sexual partners.
In this comprehensive guide, we hope to answer every question you have about female genital warts and the human papillomavirus (HPV) that causes them, including:
- Understanding The Virus That Causes Genital Warts: Human Papillomavirus (HPV)
- Everything You Need to Know About Female Genital Warts
- What Are Female Genital Warts?
- How Do You Get Genital Warts?
- How Do You Tell If It’s a Genital Wart or Not?
- What Do Genital Warts Look Like?
- What Are The Symptoms Of Female Genital Warts
- What Can Be Mistaken For Genital Warts In Females?
- Risk Factors for Developing Genital Warts
- Complications From Genital Warts
- How Do I Confirm if I Have Genital Warts?
- How Are Female Genital Warts Treated?
- Can You Treat Genital Warts at Home?
- Is Treatment Necessary for Genital Warts?
- Can Genital Warts Recur After Treatment?
- Can Female Genital Warts Be Cured?
- How To Prevent Female Genital Warts
- Genital Warts in Special Cases: Pregnancy and Children
- Other FAQs About HPV and Genital Warts
If you see a bump on or around your genitals, it is important not to use this guide to self-diagnose. It’s impossible to know if the bump you see is genital warts or something else without seeing a doctor. Attempting to Google your symptoms can create unnecessary stress, as the bumps you see might not even be genital warts.
If you notice an unusual bump on or near your vagina or a flat genital wart and live in the Nashville area, please contact Cool Springs OBGYN. Dr. Jeffery Lodge is taking new patients and can get you scheduled quickly to receive a proper diagnosis and, if necessary, discuss treatment options.
Understanding The Virus That Causes Genital Warts: Human Papillomavirus (HPV)
Before we discuss female genital warts, it’s important to have a better understanding of the human papillomavirus (HPV) that causes them. This will help you better understand how the virus works, and if warts are present, why treatment is focused on the visible warts, not the virus itself.
What is HPV?
Human Papillomavirus (HPV) is a very common group of viral infections that most adults will be exposed to and likely contract at least once in their lifetime. Not all HPV is sexually transmitted. It depends on the strain and where the virus enters the skin or mucous membranes.
Of the approximately 150-200 types of HPV that have been identified, according to the CDC, about 40 affect the genital area, as well as the mouth and throat. These strains of HPV are spread through sexual activity, including non-penetrative sexual contact like oral sex and genital touching, and are classified as sexually transmitted infections (STIs).
The remaining HPV types affect other areas of the body and are spread through nonsexual contact, often causing common, plantar, or flat warts. While rare, they can also be passed from an infected mother to her child during childbirth.
The majority of HPV infections, even those that are considered STIs, are harmless, asymptomatic and go away on their own, often without ever knowing you were infected.
However, some strains of HPV can cause physical manifestations, like genital warts, or more serious issues, like cell changes that may cause cervical cancer. The strains of HPV that cause genital warts do not cause cervical cancer.
This distinction helps explain why all genital warts are caused by HPV, but not all HPV causes genital warts. Only a few strains of HPV have the ability to cause genital warts. The same applies to cervical cancer. If cervical cancer develops as a result of HPV, only certain high-risk strains are responsible.
What is the Prevalence of HPV?
Human papillomavirus (HPV) is the most common sexually transmitted infection (STI) worldwide, with some sources stating that as many as 90% of people have HPV. However, according to the Centers for Disease Control and Prevention (CDC), that percentage is slightly lower, with the most current statistics estimating that about 85% of people will get an HPV infection in their lifetime.
Either way, those are some pretty high odds. It is more likely than not that nearly everyone will get HPV at some point in their lives. That’s the bad news. The good news is that for 9 out of 10 women, the HPV infection goes away on its own within two years, even if you contract a strain that causes genital warts.
In terms of the HPV that causes genital warts, statistics vary, but according to the CDC, approximately 13 million people in the United States become newly infected with HPV each year. Of these, approximately 340,000 to 360,000 develop genital warts.
However, over the past couple of decades, the development and widespread adoption of HPV vaccines is believed to have helped reduce the incidence of HPV-related diseases.
Is HPV Serious?
It depends on what strain of HPV you have and how well your immune system can fight off the infection, but most HPV is harmless, not linked to a serious health issue, does not have symptoms, and for 90% of women will clear up on its own within two years as the immune system fights it off.
That said, there are strains of HPV, primarily types 6 and 11, that are considered low-risk HPV and can result in clinical signs such as warts on or around your genitals, anus, mouth, or throat.
However, odds are, you will never develop visible warts. While some studies state the percentage of people with HPV who develop warts is higher, most demonstrate that only around 10% of HPV infections result in visible genital warts, despite carrying the virus.
This can obviously be both a pro and a con. Nobody wants visible warts on their genitals. However, lack of symptoms combined with how long the virus can live in the body makes it hard to know if a woman has genital warts, which can lead to the spread of the virus. This is one reason HPV is the most common STI in the United States. There are also about a dozen high-risk HPV strains that, left untreated, can lead to cell changes that can progress and lead to cervical cancer, cancer of the oropharynx (back of the throat), or another cancer of the vagina, penis, or anus.
In cervical cancer, the most common and highest risk types are HPV types 16 and 18. Low-grade changes (mildly abnormal cells) often go away on their own, just like other low-risk strains. A small percentage of persistent infections (10-20%) can cause precancerous changes called dysplasia that should be monitored or treated.
There is no single percentage for how many of the precancerous cases actually turn into invasive cervical cancer. However, we know that most regress with time, and the risk of further progression is low for most women. That doesn’t mean HPV should be minimized or that it can’t cause long-term issues. There is no blood test for HPV. For women, the most important thing they can do is have regular Pap smears.
Also, it is important to know that you can have more than one strain of HPV at the same time, meaning you could have the type of HPV that causes genital warts and the type that can lead to cervical cancer at the same time. However, the strains of HPV that can cause cancer do not cause genital warts.
Can You Cure HPV?
There is not a cure for HPV, but your immune system can typically get rid of the virus for you within a year or two. In instances where HPV causes genital warts, precancerous, or cancerous cells, the focus is on treating the physical manifestations, such as removing the warts or the abnormal cells through procedures like cryotherapy or excision.
Additionally, it’s important to understand that once your body naturally gets rid of the HPV virus, you can get it again if you are exposed to a new, different strain of HPV. You can possibly get the same strain again as well. While your immune system generally develops long-lasting, protective immunity against the specific strain you cleared, it is still possible, though considered rare, to be reinfected with the same strain later, particularly if your immune system is weakened.
Is HPV Contagious for Life?
HPV is contagious, but not necessarily for life. As long as the virus is active in the body, you are contagious, even if you do not have symptoms or were infected years ago. That means if you have genital warts, even after the warts go away, you can still have the virus and pass it on to someone else.
It also explains why genital warts often come back. While treatments can remove visible genital warts, they do not eliminate the virus from the body. This means that until the virus naturally clears, it can reactivate and cause new warts to grow in the future.
Knowing if you are still contagious is complicated. There isn’t a blood test to know your HPV status. Women can get a Pap smear that detects HPV, and if the test consistently comes back negative, it is highly likely that your body has successfully cleared the infection, and you are no longer contagious. However, for men, who can also carry HPV and have genital warts without visible symptoms, there isn’t a test that can detect HPV or confirm clearance.
It is also important to understand that even when the infection clears, the virus may remain in the body at a low level. This helps explain why you may suddenly get genital warts even if you’ve not had a new partner in a while.
Everything You Need to Know About Female Genital Warts
Caused by HPV
Now that you have a better understanding of the human pappiloma virus (HPV) that can lead to genital warts, and that only certain strains of HPV can cause them, we can get into specifics that will help you better understand if any bumps you see on or near your genitals could be genital warts or mistaken for someting else, as well as what to expect if a doctor confirms you have genital warts, and what your diagnosis and treatment options mean for your long-term health.
What Are Female Genital Warts?
Female genital warts are small, fleshy growths that can form in, on, or around the vagina after being exposed to certain strains of the human papillomavirus (HPV). Two strains of HPV, types 6 and 11, cause about 90% of all genital warts, which are sometimes referred to as “anogenital warts” in the medical community. There are other strains of HPV, such as HPV 42 and 44, that can also cause genital warts, but they are less common.
While genital warts can look different depending on where they develop, female genital warts are typically small, flesh colored, flat or slightly raised bumps that form in clusters, often described as looking like cauliflower.
However, genital warts can also appear as single pink or red bumps if they are new or they’ve become irritated. This is why many women mistake genital warts for common irritants like shaving bumps, ingrown hairs, or minor skin rashes.
Genital warts can also be confused with other warts on the skin. However, skin warts, such as flat warts, common warts, or plantar warts, are not sexually transmitted and do not typically appear on the genitals. Instead, these warts show up on other areas of the body, such as the hands, fingers, feet, or around, and sometimes in the mouth. Some are caused by an HPV strain and some are not. They are usually passed by direct contact with contaminated surfaces or through small breaks in the skin.
Additionally, HPV that causes genital warts is considered a sexually transmitted infection (STI), so there are also other STIs that can cause growths that could be mistaken a genital warts.
You might see a bump on or near your vagina, go online and type in what it looks like, and see herpes or syphilis as a possibility. Gonorrhea might even show up as a potential cause. While bumps are not a classic sign of gonorrhea, some people with gonorrhea describe having something called a nodule of gonorrhea.
A little further down, we’ll explain in more detail why any bump you see on your genitals is unlikely to be a nodule of gonorrhea, the differences between genital warts and other STIs that can cause skin growths, as well as skin conditions often mistaken for genital warts, and how you might be able to tell if a woman has genital warts.
However, it is important to remember that around 85% of sexually active men and women are exposed to HPV during their lives, but very few experience noticeable symptoms. The bumps you see might be genital warts, but statistically, they probably aren’t. Most people never develop physical symptoms after contracting the HPV strains that cause genital warts, which makes it possible to never know you have genital warts and potentially pass the virus on to someone else.
Learn about other STDs with our Ultimate Guide to STDs
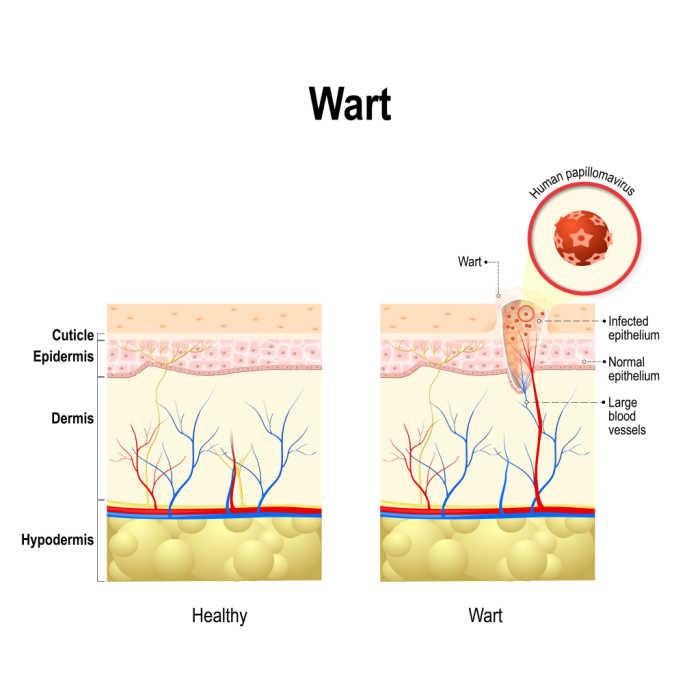
How Do You Get Genital Warts?
Genital warts are caused by specific strains of human papillomavirus (HPV). The primary way to get genital warts is skin-to-skin contact during sexual activity with an infected person. However, you do not have to have penetrative sex to get genital warts. There are other forms of sexual contact that can pass genital warts, as well as other less likely modes of transmission.
You Can Get Genital Warts From Any Type of Sexual Activity
You can contract genital warts from mucus membranes or any skin-to-skin contact with an infected person. This means that it’s possible to get genital warts from genital touching, and even if you use condoms, since they don’t cover all areas of skin where the virus can spread.
Genital warts can also potentially be spread from sharing sex toys with an infected person or if you touch yourself where there is an infected area and then touch another part of your body.
Can You Get Genital Warts From Kissing?
While rare, it is possible to get genital warts from heavy kissing, since HPV that causes genital warts can be spread through direct contact with mucous membranes, including during kissing.
However, the risk of transmission through kissing is believed to be generally low, especially if there isn’t contact with open sores or genital fluids.
Can You Get Genital Warts From Non-Sexual Activity?
There is a lot of debate about other potential ways to contract HPV, which leads people to wonder if you can get genital warts from toilet seats or sharing things like cups and utensils.
Most studies show the human papillomavirus that causes genital warts can live on surfaces for a very short period, but it is highly unlikely, as they are primarily transmitted through sexual skin-to-skin contact and mucus membranes.
However, there is a very small risk of transmission from sharing a towel if the towel is contaminated with an active infection and used shortly after, especially if there are open cuts or sores on the skin.
How Do You Tell If It’s a Genital Wart or Not?
The only way to know for sure you have genital warts is a medical exam. If you are concerned that you might have genital warts, don’t attempt to self-diagnose.
We understand that the natural reaction when noticing a bump or sore around your genitals that wasn’t there before, especially if you are sexually active and at higher risk of contracting genital warts or other STIs, is to jump online and search for answers.
However, it is impossible to determine from pictures and symptoms alone if the bump you have is genital warts. While genital warts have a few distinct features and symptoms, which we will discuss in detail next, they can resemble other common skin warts and skin conditions, such as razor burn or ingrown hairs. Additionally, there are a few other STIs that can cause skin growths or rashes.
Searching online for genital warts images or wart disease images could lead to unnecessary stress and delay proper diagnosis, and if needed, treatment. If you have a bump on or near your genitals, make an appointment with a doctor for a proper diagnosis.
What Do Genital Warts Look Like?
When genital warts caused by the human papillomavirus (HPV) are visible, they typically appear on the skin or mucus membranes of the genital area as small, closed, flat or slightly raised bumps that are skin-color, white, or pink.
Genital warts do not usually appear in other areas of the body, such as the hands, feet, or face, but they can vary in size, shape, color, and quantity. In females, genital warts can appear on the vagina (including inside the vagina and on the cervix), vulva, or vaginal lips (labia minora and labia majora). They might also be present on surrounding areas, such as the buttocks or upper inner thigh.
Genital warts can have a range of appearances, depending on factors such as the location and severity of the infection.
- Appearance: Genital warts often start as small, raised, flesh-colored or slightly pink growths that can be rough or smooth, and raised or flat. Many describe the appearance of genital warts as resembling cauliflower.
Genital warts can also be flat, making them very hard to spot. It’s important to note that flat genital warts are not the same as flat warts on other parts of the body. We will explain the distinction a little further down when we discuss common skin conditions mistaken for genital warts.
- Discharge: Unless a genital wart becomes infected, leading to a blister or sore, genital warts do not have pus or other fluid; they are typically closed. This is often one way to distinguish genital warts from other conditions. If you notice pus or fluid leaking from a bump, it could be a genital wart, but it’s more likely to be another type of infection or condition.
- Quantity: While it is more common to have more than one genital wart clustered together (often described as looking like cauliflower), it is not uncommon to have only one or two warts that may eventually grow in size or number.
- Size: Genital warts can be large, but they are generally small. In fact, in many cases, genital warts are so small that they are not visible to the naked eye and can only be detected through a physical exam or Pap smear.
- Discomfort: Typically, genital warts are painless and do not cause discomfort. While rare, sometimes genital warts can itch. They may also bleed, especially during sex.
If you notice any unusual growths or changes in your genital area, it’s best to see a healthcare provider for an accurate diagnosis and appropriate treatment. The red bumps on your butt or genital bumps you see might be genital warts, but they could also be a common skin irritant or a different sexually transmitted infection.
What Are The Symptoms Of Female Genital Warts
The symptoms of female genital warts can vary depending on the individual. Most women who carry the HPV virus that causes genital warts never develop symptoms. They may never know they even have the genital warts virus without a screening from an OBGYN.
When present, symptoms of genital warts are usually mild to moderate and may come and go over time. The most well-known symptom of genital warts is their unique appearance. There are a few other symptoms that can possibly indicate that you have genital warts.
- Flesh-colored, slightly pink, or grey growths around your vagina, anus, or upper thighs
- Cluster(s) of cauliflower-like growths
- Any bumps suspected inside the vagina
- Abnormal bleeding during or after sex
- An itchy vagina or anus
- Changes to the flow of urine
If signs and symptoms of genital warts do appear, it could be months, even years, after coming in contact with the virus. If you see a bump or bumps and suspect it might be genital warts, or have other symptoms that can sometimes be an indicator of genital warts, even if you haven’t had a new sexual partner in a long time, it’s important to see a doctor. A medical exam is the only way to know if you have genital warts.
Where do Female Genital Warts Appear?
The key locations female genital warts can grow on are the vulva, inside the vagina canal, around the vagina and anal openings, and the skin surrounding the vagina. Female genital warts can also grow inside the mouth and in the throat, if there was oral contact with the infected area.
What Can Be Mistaken For Genital Warts In Females?
Visually, several conditions may resemble genital warts. The appearance of genital warts is often mistaken for common skin conditions, such as general skin warts, flat warts, shaving bumps, ingrown hairs, or a skin tag. There are also other lesser-known conditions and STIs that can resemble genital warts.
Distinguishing genital warts from other conditions can be challenging without professional help, and you should never attempt to self-diagnose a bump on or around your genitals. That said, it can offer some peace of mind for those worried about a genital bump to have a better understanding of how to tell them apart from other skin conditions.
How to Differentiate Genital Warts from Other Skin Conditions
If you notice a bump around your genitals, statistically, it is most likely another skin condition or possibly a different STI. It is always best to schedule an appointment with an OBGYN who can give you a more definitive answer and help you take any additional steps necessary.
This guide is only to provide you with a better idea of what a bump or bumps on your genitals may or may not be.
1: Common Skin Conditions Mistaken for Genital Warts
Skin Tags
- Appearance: Small, soft skin growths that look like a tiny deflated balloon on a stalk.
- Transmission: They are not sexually transmitted and are usually harmless.
Molluscum Contagiosum
- Appearance: Viral infection causing small, round, flesh-colored bumps.
- Transmission: Can spread through direct skin-to-skin contact, similar to genital warts.
Fordyce Spots
- Appearance: Tiny, raised, yellowish, or skin-colored spots found on the genitals or other body parts.
- Cause: Enlarged sebaceous glands, not linked to STIs.
Seborrheic Keratosis
- Appearance: Noncancerous, warty growths that can be white, brown, or black, often with a “stuck-on” look.
- Prevalence: More common among older adults; not sexually transmitted.
Distinguishing Features
- Skin Tags: Typically painless and not prone to changes unless irritated.
- Molluscum Contagiosum: Tend to have a central dimple or indentation in the bump.
- Fordyce Spots: Consistent in appearance and usually do not change over time.
- Seborrheic Keratosis: Often develops a rough, bumpy texture and varies greatly in color.
2: Non-Genital Warts, Including Flat Warts
“Wart” is a common term used to describe a small growth or bump anywhere on the skin. Warts can appear anywhere on the body. Where and what they look like depends on the HPV strain and/or how they were transmitted.
Most (but not all) skin warts are caused by a type of human papillomavirus (or HPV), but not all warts are sexually transmitted or genital warts. Aside from cause, the two telling signs that a wart is a skin wart and not a genital wart are:
- Location: Common warts are on fingers, hands, elbows, or knees. Plantar warts are on the soles of the feet.
- Appearance: It depends on the type of skin wart. Most non-genital skin warts are rough, raised bumps. They often have a grayish or flesh-colored surface. Sometimes they will even have a small black dot.
We want to touch on flat warts in more detail. Because genital warts can be completely flat, many people see a flat wart on their body and become concerned that it might be sexually transmitted. While common flat warts are caused by HPV, they are not caused by the same strain that causes genital warts.
You do not have to be sexually active to get common flat warts on the skin. In fact, they are sometimes referred to as “juvenile warts” because they appear in children and teens more often than in adults.
Non-genital flat warts usually show up on the face and the top of your hands. They may also spread by shaving. For this reason, they can appear on the beard area in males and on the legs of females.
These flat warts are usually flatter and smaller than genital flat warts and also often appear in large groups, not smaller clusters, with as many as a dozen to a hundred in one area. The only similarity with genital flat warts is discomfort. Both genital flat warts and other flat warts don’t typically cause pain, but while rare, they can both itch.
3: Other STIs That Can Be Mistaken for Genital Warts
There are a few sexually transmitted infections that can cause rashes, bumps, or sores around the genitals. The two sexually transmitted infections that might slightly mimic genital warts are herpes and syphilis. However, they have very different characteristics and require distinct treatments.
- Herpes: Genital herpes often presents as painful, fluid-filled blisters rather than solid bumps. These blisters usually break open and form sores that eventually scab over. Genital herpes is not curable, but antiviral medications can reduce the severity and frequency of outbreaks and lower the risk of spreading the virus.
- Syphilis: Syphilis is a bacterial infection caused by the bacterium Treponema pallidum. It often begins as a firm, painless sore (called a chancre) that usually appears where the bacteria entered the body. If untreated, syphilis typically evolves to include a widespread rash, fever, swollen lymph nodes, and, in late stages, serious damage to organs and the nervous system. Syphilis is curable with the correct antibiotic treatment.
Other common STIs, such as chlamydia or gonorrhea, do not typically cause visible bumps or growths on the skin. However, sometimes, gonorrhea can cause other skin lesions, commonly referred to as “gonorrhea nodules”.
To the untrained eye, bumps on or around the genitals can look similar and cause unnecessary worry. An OB-GYN will easily be able to distinguish between genital warts and other infections, perform tests if needed, and recommend the proper treatment.
For more, read “I think I have an STI. What Do I Do Now?”
Genital Warts vs. Gonorrhea Nodules: A Common Misconception
Gonorrhea does not typially cause nodules or bumps. Gonorrhea is a bacterial infection that, while serious, typically presents without any visible skin growths. This STI is very different from viral HPV infections that can cause genital warts.
The classic signs of gonorhea are often asymptomatic, or symptoms like discharge and painful urination. However, while rare, it is possible to have gonorrhea and develop a nodule as part of an infection or a rare local complication.
If you have a firm bump or nodule on your genitals, it is most likely not a sign of gonorrhea. STIs that cause nodules on the genitals are more likely to be Lymphogranuloma Venereum (LGV), which is caused by a specific strain of Chlamydia trachomatis that can lead to nodules and swollen lymph nodes in the genital area. Herpes, syphilis, and even genital warts are more likely to present growths or nodules.
Importance of Professional Diagnosis
If you observe any unusual growths or changes in your genital area, consult a healthcare provider experienced in STIs.They possess the expertise to differentiate between genital warts and other conditions accurately. Early diagnosis ensures you receive the appropriate treatment, whether it’s for genital warts or another condition.

Risk Factors for Developing Genital Warts
Genital warts are usually caused by specific strains of the human papillomavirus (HPV), which spreads through direct skin-to-skin contact during sexual activity.
Here are the main factors that can increase your risk of developing genital warts:
Unprotected Sexual Activity
Engaging in sex without using condoms significantly increases the risk of HPV transmission. Although condoms provide a measure of protection, they do not fully eliminate the risk of transmitting genital warts.
Multiple Sexual Partners
Having multiple sexual partners increases your chances of being exposed to HPV. The more partners you have, the higher the risk of coming into contact with someone who has the virus, which might be a strain that causes genital warts.
Weakened Immune System
People with weakened immune systems are more at risk. Conditions like HIV or taking immunosuppressive medications can make it easier for HPV infections to take hold and for warts to persist or get worse.
Early Onset of Sexual Activity
Starting sexual activity at a young age also heightens the risk of contracting HPV. Younger individuals are more susceptible to being exposed to the virus early on.
It’s crucial to understand that while these factors increase the likelihood of developing genital warts, not everyone exposed to HPV will show visible symptoms. Some may carry the virus without any outward signs.
Complications From Genital Warts
Female genital warts can be embarrassing and cause emotional distress, but they are typically harmless and certainly not life-threatening. When properly diagnosed and treated, genital warts are usually manageable and may clear over time with the right care.
However, failing to address the underlying HPV infection that causes them can potentially cause complications. While the virus that causes genital warts (HPV) typically clears on its own within a year or two, it can cause several complications that can impact a woman’s physical and emotional health.
To help lower the risks of these complications, it is important to practice safe sex and undergo regular Pap smears that test for HPV to detect any abnormal cell changes early on and prevent the spread of HPV to your partners.
Cervical Cancer Caused by HPV
Warts are typically caused by low-risk HPV strains, like HPV types 6 and 11, and do not cause cancer. However, some strains of HPV can cause cancer, and it is possible to be infected with more than one strain of HPV.
There are several strains of HPV that might cause cancer. The highest-risk HPV strains to cause cervical cancer are HPV 16 and 18. These two strains are responsible for most cases of cervical cancer.
Even though not all types of HPV infections cause cancer, you should still get a full check-up. Having HPV and other sexually transmitted infections can also make it easier to contract HIV. This is why it’s important for women to get screened regularly as part of a preventive health care routine.
Problems During Pregnancy
In rare cases, female genital warts can cause complications during pregnancy. If the warts are present in the birth canal, they can obstruct the baby’s passage during delivery. This obstruction can lead to the need for a cesarean section to avoid harm to the baby.
We’ll discuss genital warts and pregnancy, as well as genital warts in children, a little further down.
Urinary Obstruction
If the warts are near the urethra, they may grow and obstruct urine flow, leading to discomfort and pain during urination.
Female genital warts can sometimes grow near the opening of the urethra, which is the tube that carries urine from the bladder to the outside of the body.
When this happens, the growth of the warts can obstruct the flow of urine, leading to discomfort and pain during urination. The severity of the urinary obstruction can vary depending on the size and location of the warts.
Sometimes, the obstruction may be mild, causing slight discomfort or a weak urine stream. In more severe cases, the warts can completely block the flow of urine, leading to acute urinary retention, a medical emergency requiring immediate treatment.
How Do I Confirm if I Have Genital Warts?
Noticing a new bump in your genital area can be unsettling, especially if you’re unsure what it is.
Because genital warts can look like many other harmless skin conditions, the only way to know for sure is to have a proper physical examination, and if you are female, a Pap smear at your gynecologist.
There is not a blood test that can tell you what your HPV status is, which is the virus that can cause genital warts. However, a Pap smear can detect HPV and even tell you which strains you have.
What to Expect During a Medical Exam and Testing For Female Genital Warts
Testing for female genital warts is pretty much the same as your yearly female wellness check that includes a pap smear.
During your exam, you may be asked a few questions about your symptoms and sexual history. Next, your doctor will perform a physical exam to check for warts themselves. Experienced OBGYNs, like Dr. Lodge, can identify them visually on the exterior and interior of the genitals. He will also check for hidden warts inside the vagina. This process should not be painful. Dr. Lodge handles screenings like this regularly.
The physical exam will likely be followed by a pap smear to collect cells from your cervix. This specific type of pap smear is the only test for the human papillomavirus (HPV) that causes genital warts. It checks for all strains of HPV, including the ones that can cause genital warts and cervical cancer.
How Are Female Genital Warts Treated?
While treatment for genital warts doesn’t eliminate the human papillomavirus (HPV) itself, if you have genital warts, the bumps themselves are treatable. Treatment options include topical medications, cryotherapy (freezing), laser surgery, and electrosurgery.
In this section, several treatment options will be covered for female genital warts. Some methods may be more effective than others, depending on the size and location of the warts. Visible warts on the outside of your body are easier to treat.
Cryotherapy for Female Genital Warts
Cryotherapy is a standard treatment for female genital warts. A healthcare provider uses liquid nitrogen to freeze and destroy the warts during this procedure.
The extreme cold causes the warts to peel off over time. Cryotherapy is often effective for small to medium-sized warts and is relatively quick and straightforward. However, complete removal may require multiple treatments.
Laser Surgery for Female Genital Warts
Laser surgery is another option for treating genital warts. This procedure uses a focused laser beam to vaporize and remove the warts. Laser surgery is precise and can target warts in delicate areas with minimal damage to surrounding tissue.
Laser surgery is often recommended for larger or hard-to-reach warts. Recovery time is typically shorter than other treatments, but may require multiple sessions.
Electrosurgery for Female Genital Warts
Electrosurgery, or electrocautery, involves using an electrical current to burn and remove genital warts. This method can be effective for warts of various sizes and locations. It’s a quick procedure that cauterizes the warts, helping to stop bleeding and reduce the risk of infection.
However, there may be some discomfort during the process, and multiple sessions may be necessary for complete wart removal.
Topical Medications for Female Genital Warts
Topical medications can treat genital warts, especially in cases where warts are small and widespread. However, topical treatments are generally less invasive than cryotherapy, laser surgery, or electrosurgery.
These medications typically contain chemicals that work to destroy the warts over time. Some examples of topical treatments include:
- Podofilox: Podofilox is a gel or solution-based dosage available through a doctor’s prescription, used to treat warts between the genitals and rectum.
- Imiquimod: Imiquimod is a cream-based dosage available through a doctor’s prescription and applied to help your body fight the viruses that cause warts.
- Trichloroacetic acid (TCA): Trichloroacetic Acid (TCA) is a chemical solution applied by a professional healthcare provider that kills the proteins of genital wart cells.
Through repeated use, warts will gradually decrease in size and eventually disappear. Applying these medications requires strict adherence to a healthcare provider’s instructions, and visible results may take several weeks. Know that these treatments do not cure HPV infection.
Things To Avoid During Genital Wart Treatment
During treatment for genital warts, avoid irritating soaps and lotions. Having intercourse may also irritate the skin, and it is best to avoid that until treatment is finished. It may take several weeks for a genital wart treatment to be effective, depending on the type of treatment.
Can You Treat Genital Warts at Home?
Genital warts are different from warts on the hand or feet. Do not try an over-the-counter remedy for these areas, or attempt to remove warts from the genital area yourself. This could damage the delicate skin in the genital region.
Dr. Lodge, an experienced OBGYN in Cool Springs, TN, can prescribe the best course of treatment that won’t harm your skin.
Is Treatment Necessary for Genital Warts?
In most cases, treatment is unnecessary if your genital warts are small and you don’t have any severe symptoms. However, you may want to treat genital warts for cosmetic reasons, as they may be embarrassing.
If you or your doctor decides to treat your genital warts, they are usually easier to treat if you begin treatment as soon as you notice them.
Can Genital Warts Recur After Treatment?
Yes, genital warts can recur even after treatment. The primary reason for this is the persistence of the human papillomavirus (HPV) in the body. Although treatments can remove visible warts, they don’t eliminate the virus entirely.
How to Manage the Recurrence of Genital Warts
While genital warts can recur, taking proactive measures and working closely with healthcare providers can help manage and reduce the risk.
- Regular Follow-Ups: It’s crucial for individuals who have had genital warts to schedule regular check-ups with their healthcare providers. This helps in the early detection and management of any recurring warts.
- Preventive Measures: Adopting preventive strategies, such as using barrier protection during sexual activities, can significantly reduce the risk of recurrence.
- How can I prevent genital warts?
- To prevent contraction of genital warts, you should receive the HPV vaccine, limit the number of partners you have, and use protection. Using protection, like a condom, does not guarantee protection from genital warts, but it can lower your chances.
- How can I prevent genital warts?
- Healthy Lifestyle: Maintaining a robust immune system through a healthy lifestyle, including a balanced diet, regular exercise, and avoiding smoking, can help the body fight off HPV more effectively.
Will Genital Warts Go Away?
Your body is capable of getting rid of genital warts naturally. But if they do not resolve on their own, topical medications, cryotherapy (freezing), laser surgery, and electrosurgery are available to you at Cool Springs OBGYN.
Can Female Genital Warts Be Cured?
The good news is that warts themselves can be treated and removed. Some cases of genital warts will resolve on their own over time, but they cannot be guaranteed to go away entirely without treatment.
Unfortunately, there is no medical cure for the human papillomavirus (HPV) itself. Some people’s bodies are able to clear the virus naturally over time. You will need screenings to confirm if the virus is still active in your body.
There is no such thing as a mild case of genital warts in men or women. If you see the wart or have tested positive for the virus, you have the STI and may be able to transmit it.
How To Prevent Female Genital Warts
As genital warts are a sexually transmitted infection that can be passed from person to person through skin contact, they can be hard to prevent.
There is no sure way to prevent genital warts, and sexually active people are at risk, but there are several steps you can take to reduce your risk of exposure:
- Get vaccinated against HPV. The HPV vaccine is a very effective way to protect yourself against the virus that causes genital warts.
- Get regular screenings for HPV and other STIs for early detection and management of HPV-related conditions.
- Use condoms and dental dams every time you have sex or oral sex.
- If sharing sex toys, make sure they too are covered in a condom and washed between use.
- Avoid skin-to-skin contact with someone who has genital warts. (Remember that even after treatment, the virus can still be passed up to 3 months after warts have been removed.)
- Reduce the number of sexual partners to lower your overall risk of exposure to genital warts.
It is also important to have open and honest communication with your partner(s) about your and their sexual health.
Genital Warts in Special Cases: Pregnancy and Children
If you are pregnant and concerned you might have genital warts, or know you have them and are concerned about passing them on to your child, you likely have specific questions about genital warts. You might also have questions if you have a child who has warts and have concerns that they could be genital warts.
Here is a breakdown of what you need to know, based on medical facts.
General Warts and Pregnancy
What Causes Genital Warts During Pregnancy?
Genital warts that appear during pregnancy are caused by the same low-risk strains of HPV that cause them at any other time (primarily types 6 and 11). The infection occurs by contracting HPV either before or during the pregnancy.
The primary difference is that due to hormonal and immunological changes, warts may grow more quickly, become larger, or multiply during pregnancy. Conversely, they may also spontaneously resolve.
Can You Treat Genital Warts While Pregnant?
Treating genital warts during pregnancy is possible during pregnancy, but it is often postponed unless the warts are large enough to obstruct the vagina or make urination difficult.
Many common topical treatments for genital warts are restricted during pregnancy, as their effects on the fetus are unknown or considered harmful. Should your doctor decide your genital warts need to be treated, safe treatments typically include:
- Cryotherapy: Freezing the warts with liquid nitrogen.
- Surgical Excision: Cutting the warts away.
- Trichloroacetic Acid: A chemical solution applied by a doctor.
Risk of Genital Wart Transmission to a Baby
The risk of transmitting HPV to your baby during a vaginal delivery is low. In the rare event that transmission occurs, the virus may cause recurrent respiratory papillomatosis (RRP) in the child, which involves warts growing in the throat or lungs.
A Cesarean section (C-section)is rarely necessary for the prevention of RRP. It is generally reserved for cases where the warts are so large and widespread that they would physically block the birth canal, which is highly uncommon.
Genital Warts in Children
Are Genital Warts Common in Children?
Skin warts are common in children, but genital warts are rare. When they do occur, proper diagnosis is crucial because their presence can be alarming and requires careful medical evaluation.
How Do You Treat Genital Warts in Children?
Treatment in children must be done under the supervision of a pediatric specialist or a healthcare provider with expertise in this area, as the skin is much more delicate and sensitive. Treatment options may include:
- Cryotherapy
- Excision
- Specific low-concentration topical medications
Non-Sexual Genital Wart Transmission vs. Abuse
While the appearance of genital warts in a child may indicate sexual abuse and must always be thoroughly investigated, it is medically important to know that non-sexual transmission is also possible. The virus can sometimes be spread through non-sexual contact (e.g., from a caregiver’s hands to the child’s genitals) or through HPV present during birth.
Because of these possibilities, a definitive diagnosis and an investigation by healthcare and social service professionals are essential.
Other FAQs About HPV and Genital Warts
Do Genital Warts Itch?
Genital warts are typically painless, but in some cases, they can cause symptoms such as itching, burning, or discomfort, especially if they are irritated by friction. Bleeding after sexual intercourse is also possible.
How Long Do Genital Warts Last?
For many people, the HPV infection that causes genital warts clears spontaneously, and the warts will go away on their own within two years. However, in other cases, they can persist, with many choosing medical treatment to remove the visible growths. Even after treatment, warts can recur, as the underlying virus may still be present.
Will genital warts go away?
Yes, genital warts can naturally go away, but if they don’t resolve by themselves, then alternative treatment is available.
Can Genital Warts Be Completely Flat?
Yes, genital warts can be completely flat. Genital warts are much harder to spot than raised warts. They may appear flush with the skin or mucous membrane, particularly when found on the cervix or inside the vagina.
Do Flat Warts Mean I Have HPV?
Yes, if a bump is definitively diagnosed as a flat genital wart (or any genital wart), it confirms that you have been infected with one of the low-risk strains of the Human Papillomavirus (HPV).
How Do You Know If A Woman Has Genital Warts?
Unless a woman has had a pap smear that confirms HPV, the virus that causes genital warts, or visible growths that are confirmed to be genital warts, you can’t look at someone and know if they have genital warts.
Sometimes warts are present, but often they are not. A person can have HPV that causes genital warts and not have any visible warts or other symptoms.
Is Genital Warts a Bad STD?
Genital warts are generally considered a low-risk sexually transmitted infection (STI), not a severe sexually transmitted disease (STD). Most medical professionals now use STI because the HPV infection often clears up without ever causing a “disease” (or symptoms).
The strains of HPV that cause genital warts (primarily types 6 and 11) are different from the high-risk strains that cause cancer. While they are a nuisance, they do not pose a serious risk to your heart or of progressing to cancer.
Schedule an STI Screening for Genital Warts in Cool Springs, Tennessee
If you are experiencing any of the symptoms associated with female genital warts, it is important to seek medical treatment as soon as possible. It is also important for women who are sexually active to be screened for HPV on a regular basis, especially if they have multiple sexual partners.
Please fill out a form online or give the staff at Cool Springs OBGYN in Brentwood, Tennessee, a call to make an appointment. Call us at 615.690.6600, Monday through Thursday, for women’s health care with all the latest advances in gynecology.